I believe that everyone can find something for themselves here. If diabetes affects your life personally, remember that this blog does not provide medical advice and recommendations on how to manage this chronic, incurable disease. Every diabetes case is unique. There is no universal best treatment, best technology, or best approach. Always consult with a qualified healthcare provider for the management of your or your child’s specific diabetes case.
Mia, a 5-year-old first-grader, couldn’t read or write when she began school. Six months after being diagnosed with type 1 diabetes, she was expected to spend most of the day away from home, without us. However, regardless of how difficult it was for me to envision, I didn’t allow my worries and fears to shape her future.
School, school clubs, snacks during every break, and lunch with siblings – all of these pose significant challenges for families managing diabetes.
The following shared experiences assume that you are using a CGM (Continuous Glucose Monitor) to help you manage your child’s diabetes.
With school ahead, how can you prepare to handle it effectively?
1. Insulin pump with a closed loop

What did this step mean for us? It meant the end of 4-5 or more daily injections for our child, the end of using two types of insulin and carrying pouches with pens/syringes, the end of worries about their proper storage, the end of fear about insulin mix-ups, and, above all, the end of our child’s dependence on us as parents/caregivers.
In insulin pumps, faster-acting insulin is typically used in Slovakia compared to the standard fixed regimen, which simplifies diabetes management. It’s true that changing established routines from slower insulin may not be easy, but it takes time to adapt to each ‘new thing.’ Remember, even using the most super-advanced system has a learning curve; it will require your effort. It doesn’t mean you can forget about your child’s type 1 diabetes, but from my perspective, mastering it correctly makes life easier for the child and the whole family.
How to choose a pump and why go for a closed loop? When it comes to choosing a pump, I’d recommend selecting one that complements a sensor that works well for your child. However, this doesn’t mean a different or new sensor won’t be suitable. Choosing an insulin pump is a significant decision that typically commits you for several years in most countries. Take your time with this decision, but also be open to making compromises if needed. Consult with your doctor, meet with dealers who offer various pumps on the market, and let them explain why their product is the right choice for you. For pumps with tubes, it’s also a good idea to try different types of cannulas beforehand. I highly recommend it.
Closed loop systems – these work by having the sensor communicate with the pump, providing real-time information about the user’s current blood glucose levels. Based on this data, the algorithm makes decisions about whether to decrease, maintain, or increase insulin delivery to keep blood glucose within the target range. These automated decisions significantly simplify daily life with diabetes for you or your child. The system operates based on parameters you set and the blood glucose readings from the sensor, making these two elements the foundation of successful diabetes management.
The available CGMs in Slovakia include:
- Guardian – compatible with Medtronic pumps.
- Dexcom G6 – compatible with Tandem pumps.
- Libre 2 as a CGM (available from October 1, 2023)- it is not officially compatible with any commercial pumps in Slovakia, however, you shouldn’t exclude it from the game at first sight.
In practice, you have these three options. You can discuss your choice with your diabetologist and the dealers of these medical devices.
Now that Libre 2 CGM is available your choice enlarged of setup with a Dana pump (available in Slovakia), some Accu-Chek pumps (it’s going to be out of market soon, some old versions of Medtronic pumps, and others that are not commonly found in Slovakia (like Omnipod).
In Europe, the most commonly used “off-label” system for connecting communication between sensors and pumps is AAPS. It’s an application that you build yourself from open source, but it comes with certain responsibilities. It requires your full commitment, access to a computer, and basic technical skills. Due to these requirements, it’s not a common or first-choice option. AAPS allows users to combine various CGMs and insulin pumps for personalized diabetes management. You can find more details about AAPS here.
Other open-source applications include Loop (for Apple users), iAPS (Apple and Android users), and Open APS. Each of these has its unique features and functions differently, although some aspects may overlap. You can find more details about Loop here, Open APS here and iAPS here.
In simple terms, if for any reason you choose to go “off-label” (meaning using a system that’s not officially approved or certified for diabetes management), you should consider either AAPS or Loop for your child. AAPS is suitable for Android phone and Windows users, while Loop is designed for Apple iPhone and you can build it on any computer. Once you’ll become experienced user, you can experiment with other DIY APPS.
2. Remote Monitoring of Your Child
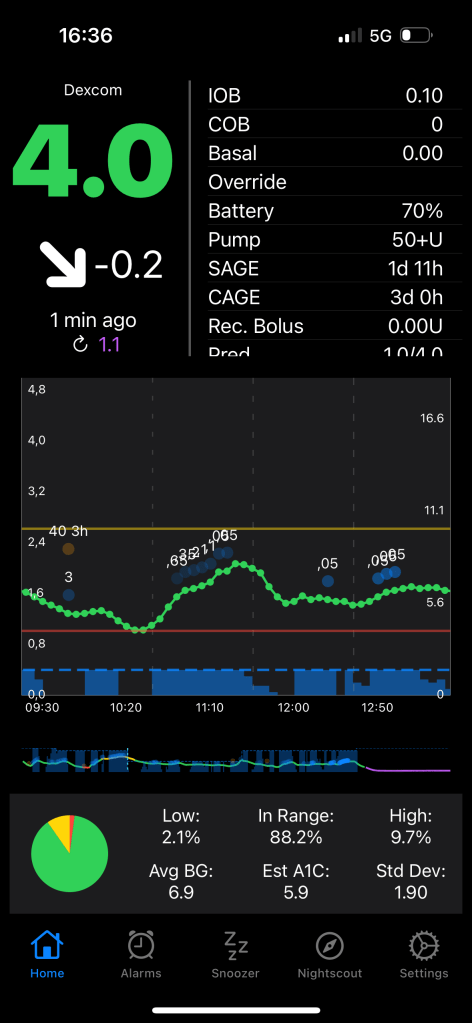
I haven’t used commercial closed-loop systems myself, but let me explain what gives me peace of mind when my daughter is not with me and what options I have. Currently, we’re on the Loop & Omnipod & Dexcom G6 combo).
Here are some things you can monitor:
- What and when your child ate (g of carbs).
- Whether they administered the correct bolus insulin dose for their meal.
- Whether the pump is running in automatic mode (closed-loop).
- Any automatic corrections made through basal or bolus insulin.
- Whether your child is using any predefined mode, such as for sports.
- Additional helpful features include glucose level predictions, the battery status of your child’s phone and when to change the pump/cannula, sensor session expiration.
- Information on insulin and carbohydrates on board.
When it comes to commercial systems, they provide valid options, but their advancements for remote monitoring can vary. It’s essential to consult with representatives to understand the capabilities of offered products. Also, consider whether your child uses an iPhone or Android, as this can affect your available options, which may be more limited in some cases – countries.
The mentioned off-label options like AAPS and Loop (iAPS as well) also provide you, parent or caregiver, the ability to remotely manage your child’s diabetes. This means you can administer bolus insulin, input carbohydrates, and switch to temporary overrides from anywhere in the world. This can be highly beneficial, not only when caring for a child with special needs.
3. Independence
The independence of a child, and especially our ideas about their independence, is a very sensitive issue. The age of the child plays an important role, for example, at the age of 2-3, they can’t manage themselves even with a closed loop system. Another crucial factor is the temperament and parenting style. It’s highly individual, and each family makes different decisions. Some parents expect their children to be capable of making fingerpicks to check their glucose levels, administering insulin injections, replacing sensors from a very early age.
On the other hand, some parents assume a significant portion of the daily diabetes management responsibilities for their children, often continuing into their children’s adulthood.
Please, let’s try not to judge or evaluate what may seem right to us. Being constantly under significant psychological pressure is very demanding for all of us.
What I believe a 5-year-old child can handle without major difficulties, and how we started:
Pictures and numbers – a picture of fruit, bread, and a number (g of carbs) that needs to be entered. It’s good if, at the beginning, an adult checks whether the child is entering the numbers correctly. Although I had concerns before, a 5-year-old child can handle this task cleverly. If you have some time to practice during the summer holidays before school starts, you’ll be calmer in September. Your child can easily manage this with your trust. What if they make a mistake? Let’s not pretend that it never happens to us 🙂 Rule number one; no panic. When you are prepared for all possible situations, you will find it easier to deal with them when they occur. In any case, let’s try not to transfer our fear to the little ones and teach them that they can handle every situation. If not, it’s okay to ask for help.
What should a child learn? It’s good if the child learns to enter a number (g of carbs) and confirm the bolus before they start eating. If they make a mistake, teach them how to correct entered carbohydrates (if you have this option). If they enter the number twice, teach them how to delete the carbohydrates (if you have this option). If you think they won’t eat their lunch, split the number in half, and if they eat everything, they can enter the second half after the meal. I put a sticker on a water bottle. (It’s always good to remind them in the morning to at least eat half). Cookies or some complex carbs for every situation in the backpack is not a bad idea, too.
If an alarm starts during school activity, and you already know about it, you can teach your child how to turn off the alarm (if possible) until you arrive. A 6-year-old child, depending on their skills, can already handle basic tasks related to operating the pump. Turn it off, fill, prime stick it… We don’t turn it into a routine for now; rather, we teach it as a way to handle emergencies or sleepovers.
After I found that numbers and drawn pictures worked well for us, I decided it was time for Mia not to have to call me every time when I’m not with her or she’s at a sleepover, in the cinema… and she’s going to eat. So, I made her cards. With favorite treats or the most common meals, she could have carbohydrates with her meals anytime, anywhere, as needed. The cards can also be a helpful tool for another adult in the family or whoever is taking care of the child at that moment. However, in our case, I always deal with things related to her diabetes management only with Mia. (But you probably know that the fewer third parties involved, the better).
Laminated cards, palm-sized, can fit anywhere, in a pocket, a mobile phone pouch, a school bag, a favorite backpack; they won’t take up space even at grandparents’ or in a cottage… at the beginning, we had them everywhere. A child will quickly learn and remember the numbers of their favorite sweets, meals; over time, the cards will be stored among their favorite pictures on their mobile. At first, it might be challenging to have only pictures on the mobile because a first-grader won’t immediately remember which number corresponds to which food when they need to enter it, for example, on their phone, while using Loop for example.

For the cards, it’s easiest to use emojis; for children are easy-peasy. The number next to bacon represents additional carbohydrates from fats and proteins (fat-protein units). I found the widely used calculation formula to work for us: 30% of total fats + proteins – fiber. You should know or consult with your diabetologist about fat-protein units. The bold number represents the number of grams of carbohydrates.
Living with type 1 diabetes presents ongoing challenges, but your children will lead joyful and fulfilling lives if you support their path to independence. Am I entirely fearless? Certainly not! Which parent is? However, it’s crucial to understand that our fear can’t impede their growth and pursuit of their dreams, with or without diabetes. So, you shouldn’t allow anxiety to restrict them either. I do believe our determination can truly make all the difference.
You can follow Mia and her adventures on Instagram account @miatype1dmaniacdaugther.



